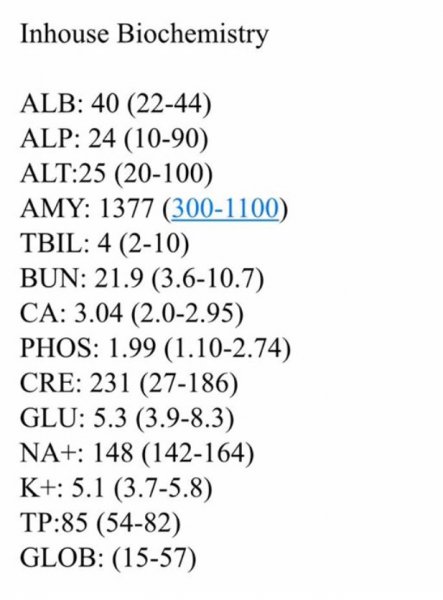
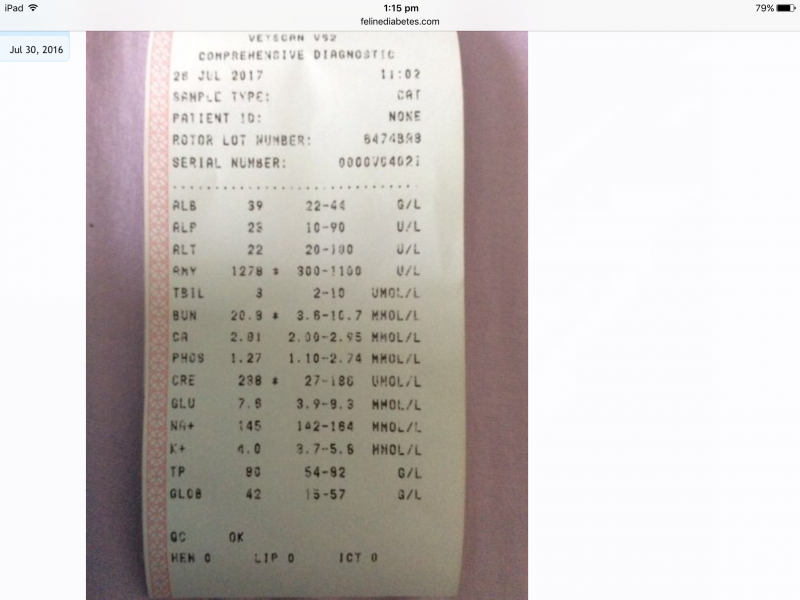
No issue with aluminium toxicity? Some articles I read mentioned this.
From the above mentioned page:
Aluminium Toxicity
You may have read that there is a risk of aluminium toxicity from the aluminium in aluminium hydroxide medications. This applies in particular to human patients on dialysis, because aluminium is used in the dialysis process.
Do aluminium hydroxide binders continue to have a role in contemporary nephrology practice?(2011) Mudge DW, Johnson DW, Hawlet CM, Campbell SB, Isbel NM, van Eps CL & Petrie JJB
Nephrology 12 states "Available historical evidence however, suggests that neurological toxicity may have primarily been caused by excessive exposure to aluminium in dialysis fluid, rather than aluminium-containing oral phosphate binders. Limited evidence suggests that aluminium bone disease may also be on the decline in the era of aluminium removal from dialysis fluid, even with continued use of aluminium binders...The relative contribution of aluminium binders to aluminium toxicity would appear to be minor based on the available evidence."
Do oral aluminium phosphate binders cause accumulation of aluminium to toxic levels?(2011) Pepper R, Campbell N, Yaqoob MM, Roberts NB & Fan SLS
BMC Nephrology 12 found that even patients on dialysis did not develop aluminium toxicity if changes were made to the dialysis process (during which patients may be exposed to dialysate water which is contaminated with aluminium), but the patients in this study were on relatively low doses of aluminium hydroxide.
Since cats are not on dialysis, aluminium toxicity was not thought to be a concern for cats (or dogs), especially since even in humans it takes years before it becomes a problem, and cats and dogs don't live as long as humans. Recently, however, there has been increasing concern about the possible risk of aluminium toxicity in cats using aluminium hydroxide based binders. This is partly because of a study which reported on aluminium toxicity in two dogs on binders,
Aluminum toxicity following administration of aluminum-based phosphate binders in 2 dogs with renal failure (2008)
Segev G,
Bandt C,
Francey T &
Cowgill LDJournal of VeterinaryInternal Medicine 22(6) pp1432-5. There is no abstract available for this study, but
Treatment options for hyperphosphataemia in feline CKD: what's out there?(2009) Kidder AC & Chew D
Journal of Feline Medicine & Surgery 11(11) pp813-24 reported that the two dogs in question developed "probable aluminum toxicity" after being on binders for only 62 and 65 days. The symptoms seen were "severe neuromuscular abnormalities." The dogs were on dosages of 125mg/kg per day (or 56mg per lb body weight) and 200 mg/kg (or 91mg per lb bodyweight) per day, which are not particularly high doses. However, both these dogs had been on dialysis, though apparently the dialysate water was not contaminated with aluminium.
Partly because of this study, vets are becoming increasingly aware of the need for caution and awareness when using aluminium hydroxide binders in cats too, particularly when using large doses. In
Chronic kidney disease (CKD) in dogs and cats - staging and management strategies (2015)
A Presentation to the Virginia Veterinary Medical Association 2015 Virginia Veterinary Conference, Dr D Chew says "THERE IS NO KNOWN SAFE DOSE OF ALUMINUM SALTS FOR HUMANS WITH CKD. Detrimental effects of aluminum based phosphate binders as described in humans seen in humans have not been systematically evaluated in small animal patients and are rarely clinically appreciated. As cats with CKD can live for years on treatment, concerns for aluminum accumulation deserve more study as to long-term safety."
Physical symptoms to watch for include muscle weakness or neurological problems, such as stumbling and an awkward gait (although, just to complicate matters, these can actually be signs of uncontrolled phosphorus levels too, see
above). One possible early sign of aluminium toxicity is a change in
MCV. This is a measure of red blood cell size. If your cat has a low MCV (known as microcytosis), this means the red blood cells are smaller than usual. Although this may simply indicate iron deficiency, it may also be a sign of aluminium toxicity. This sign normally appears before you see physical symptoms, so be sure to monitor your cat's MCV levels.
If you are using
potassium citrate (perhaps to treat
metabolic acidosis), give this at least two hours apart from phosphorus binders. This is because, as
Drugs explains, products containing citrate can in theory increase the absorption of aluminium, which could increase the risk of aluminium toxicity. Many therapeutic kidney diets contain potassium citrate. See
above for more information on aluminium hydroxide and potassium citrate.
Try not to worry too much. I am only aware of one case of aluminium hydroxide toxicity in cats to date (this cat was given massive doses of aluminium hydroxide, more than twice as much as she would normally be given based upon Dr Nagode's table above), and most cases in dogs have occurred in dogs taking over 200 mg/kg. In
Updates in feline chronic kidney disease (2008) Dr CL Langston states "Excessive absorption of aluminum can lead to toxicity, including anemia and neurologic symptoms, but this seems uncommon in veterinary practice." In contrast, the dangers of elevated phosphorus control are very real, and very common, and controlling phosphorus is essential for your cat's wellbeing.
If your cat has phosphorus levels that require large amounts of aluminium hydroxide, or if you cannot control your cat's phosphorus levels with aluminium hydroxide only, consider adding another phosphorus binder. Most people in this situation use lanthanumcarbonate (Renalzin or Fosrenol). See
below for suggestions on dosage.
If you think your cat may have aluminium toxicity, I would ask for a referral to a vet school or a neurologist if possible. Chelation therapy plus dialysis helped to remove the aluminium from dogs with aluminium toxicity, and indeed following treatment the neurological problems experienced by the dogs in the above study were successfully reversed.